- New stuff to read and discuss
- What patients say
- Clinic / online appointments
- Why the diagnosis of a psychosomatic illness is often a misdiagnosis
- Vascular Compression Syndromes
- Do you have questions?
- Checklist vascular compression syndromes
- Description of your symptoms
- Researchers from the Mayo Clinic confirm my concept of the Midline Congestion Syndrome
- Explanation of gender-specific differences in the clinical symptoms of abdominal vascular compression syndromes: varicocele and penile/testicular pain – their main manifestation in men.
- Varicocoele is predominantly caused by left renal vein compression
- Musculoskeletal pecularities of female puberty
- Lordosis /Swayback- Origin of many abdominal compression syndromes
- Bending of a straight vein compels its narrowing
- The lordogenetic midline congestion syndrome
- Neurological consequences of the midline congestion syndrome
- Successful treatment of a teenage girl who was unable to eat due to extreme postprandial pain and unable to walk due to spasticity in her left leg
- Severe ataxia in a young woman with severe spinal congestion – complete resolution after decompression of the left renal vein
- All compression syndromes are one: the spectrum of lordogenetic compressions
- Nutcracker-Syndrome is a misnomer! Lordogenetic left renal vein compression is a more appropriate name!
- May-Thurner-constellation (May-Thurner-syndrome, Cockett’s syndrome)
- Midline (congestion) syndrome
- Pelvic congestion syndrome
- Celiac Trunk Compression / Dunbar syndrome / MALS / Arcuate ligament syndrome
- Wilkie-Syndrome / Superior-mesenteric-artery-syndrome
- Compression of the vena cava inferior
- Evlauation of vascular compressions with the PixelFlux-method
- Connective tissue disorders predispose to multiple compressions
- Postural tachycardia syndrome (POTS) – the hemodynamic consequence of vascular compression syndromes and loose connective tissue
- Restless legs-a little known symptom of abdominal vascular compression syndromes
- Pudendal neuralgia in vascular compression syndromes
- A new sonographic sign of severe orthostatic venous pooling
- Migraine and Multiple Sclerosis
- Hemodynamic effect on cerebral perfusion in patients with multiple localised vascular compression.
- Treatment of vascular compression syndromes
- Fatal errors in the treatment of vascular compression syndromes
- Risks of stents in venous compression syndromes
- Surgical treatment of abdominal compression syndromes: The significance of hypermobility‐related disorders
- Nutcracker and May-Thurner syndrome: Decompression by extra venous tube grafting and significance of hypermobility related disorders
- Our surgical treatment of vascular compressions
- Chronic regional pain syndrome (CRPS) caused by venous compression and mechanical irritation of the coeliac plexus
- Vascular compression syndromes and other disease mechanisms I recently detected
- Kaleidoscope of instructive cases
- Venous congestion of the spinal cord may be a potential contributor to the development of paraplegia in patients with spinal muscular atrophy type III (Kugelberg-Welander disease)
- Ultrasound Diagnostics
- A breakthrough in functional sonographic diagnostic – 4D-colour Doppler sonographic flow volume measurements
- 4D-volume flow measurements of jugular and mesenteric veins
- Inauguration of the global volumetric brain perfusion measurement-a gateway for understanding of neurological symptoms
- Ultrasound focused entirely on all of your symptoms
- Ultrasound vs. X-ray
- Vascular Malformations
- Profile
- Functional colour Doppler ultrasound – how I do it
- Perfusion Measurement – PixelFlux-method
- Research
- Publications
- Nutcracker and May-Thurner syndrome: Decompression by extra venous tube grafting and significance of hypermobility related disorders
- Papers authored by Th. Scholbach
- Publications
- Inauguration of measurements of the tissue pulsatility index in renal transplants
- From nutcracker phenomenon to midline congestion syndrome and its treatment with aspirin
- First sonographic tissue perfusion measurement in renal transplants
- First sonographic bowel wall perfusion measurement in Crohn disease
- First sonographic renal tissue perfuison measurement
- First sonographic measurement of renal perfusion loss in diabetes mellitus
- PixelFlux measurements of renal tissue perfusion
- Why I prefer not to publish in journals but in the Internet
- Vessel stretching in nephroptosis – an important driver of complaints
- Publications
- Expertise
- Bornavirus Infection
- Scientific cooperation
- Cookie Policy
- Data protection
- Cookie Policy (EU)
- Impressum

Posture dependent unbearable breathlessness and fullness in the right upper abdomen due to a variable diaphragmatic compression of the hepatic veins and the vena cava inferior
The patient, a slender woman of 65 years, suffers from breathlessness and massive tension and fullness in the right upper abdomen as soon as she needs to bend forward or lies on her left side. This developed after a bicycle accident 3 years ago when she fell on her right sided thorax. 7 years ago she was operated on recurrent pneumothoraces on the right side for which a pleural endometriosis was found being responsible.
After this operation no problems with breathing occurred until the accident 3 years ago.
A repeated CT of the thorax, an MRI of the trunk and abdomen as well as ultrasound of the abdomen did not reveal any cause of her complaints. Since she also wakes up at night sweating breathless and with tachycardia and arrhythmia her symptoms finally have been classified as psychosomatic. She is desparate since she cannot work in a hotel anymore where she needs to cover beds requiring a bending forward.
The ultrasound examination of the liver and its vessels but demonstrated a reason for her complaints. The diaphragm was compressing the mouth of the hepatic veins as well as the vena cava inferior as soon as the patient assumed those positions which were very unpleasant and caused her breathlessness.
This was bending forward while being upright (sitting or standing) and lying horizontally on her left side. Then a massive flow acceleration within the confluence of the hepatic veins could be demonstrated up to more than 310 cm/s whereas in the central portions of the liver veins the flow velocity was as low as 13 cm/s.
 A similar flow acceleration was found in the vena cava inferior due to its compression by the diaphragm.
A similar flow acceleration was found in the vena cava inferior due to its compression by the diaphragm.
Moreover, the liver was found compressed by 2 ribs which squeezed the right liver lobe when the patient was bending forward impressing its surface by 14 mm. This liver compression was also affecting the compression of the vena cava inferior.
The liver was also slightly swollen with a height of 16.6 cm (normal less than 13 cm).
Since the patient also had slightly elevated liver enzymes (ALAT) a low-grade liver damage by the above-mentioned mechanisms can be assumed since conventional reasons for elevated liver enzymes as infections or toxic damages had been ruled out.
The pleura of the right lung was unremarkable during the sonographic examination.
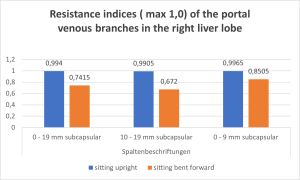
The tenderness and fullness in the right hypochondrium is explained by the suddenly increasing tension of the liver due to the posture-dependent venous congestion of this organ. This could be demonstrated by liver parenchyma perfusion measurement with the PixelFlux technique. The small subcapsular branches of the portal vein showed a high pulsatility and reduced venous volume as long as the patient was comfortable while being upright or lying horizontally on her back. This points to an easy passage of portal blood via the liver parenchyma to the hepatic veins since their outflow was only little constricted by the diaphragm.
When she provoked her symptoms by turning to her left side while lying horizontally or bending over while sitting her symptoms with breathlessness and fullness in the right hypochondrium developed within seconds while the parenchymal liver veins dilated and became congested.
Their pulsatility was suddenly reduced since the sudden massive congestion did not allow a rhythmic outflow via the liver veins anymore.
This sudden blockage of flow from the lower hemisphere to the heart explains the posture-dependent tachycardia and arrhythmias and may contribute to breathlessness due to a suddenly reduced lung perfusion.