- New stuff to read and discuss
- What patients say
- Clinic / online appointments
- Why the diagnosis of a psychosomatic illness is often a misdiagnosis
- Vascular Compression Syndromes
- Do you have questions?
- Checklist vascular compression syndromes
- Description of your symptoms
- Researchers from the Mayo Clinic confirm my concept of the Midline Congestion Syndrome
- Explanation of gender-specific differences in the clinical symptoms of abdominal vascular compression syndromes: varicocele and penile/testicular pain – their main manifestation in men.
- Varicocoele is predominantly caused by left renal vein compression
- Musculoskeletal pecularities of female puberty
- Lordosis /Swayback- Origin of many abdominal compression syndromes
- Bending of a straight vein compels its narrowing
- The lordogenetic midline congestion syndrome
- Neurological consequences of the midline congestion syndrome
- Successful treatment of a teenage girl who was unable to eat due to extreme postprandial pain and unable to walk due to spasticity in her left leg
- Severe ataxia in a young woman with severe spinal congestion – complete resolution after decompression of the left renal vein
- All compression syndromes are one: the spectrum of lordogenetic compressions
- Nutcracker-Syndrome is a misnomer! Lordogenetic left renal vein compression is a more appropriate name!
- May-Thurner-constellation (May-Thurner-syndrome, Cockett’s syndrome)
- Midline (congestion) syndrome
- Pelvic congestion syndrome
- Celiac Trunk Compression / Dunbar syndrome / MALS / Arcuate ligament syndrome
- Wilkie-Syndrome / Superior-mesenteric-artery-syndrome
- Compression of the vena cava inferior
- Evlauation of vascular compressions with the PixelFlux-method
- Connective tissue disorders predispose to multiple compressions
- Postural tachycardia syndrome (POTS) – the hemodynamic consequence of vascular compression syndromes and loose connective tissue
- Restless legs-a little known symptom of abdominal vascular compression syndromes
- Pudendal neuralgia in vascular compression syndromes
- A new sonographic sign of severe orthostatic venous pooling
- Migraine and Multiple Sclerosis
- Hemodynamic effect on cerebral perfusion in patients with multiple localised vascular compression.
- Treatment of vascular compression syndromes
- Fatal errors in the treatment of vascular compression syndromes
- Risks of stents in venous compression syndromes
- Surgical treatment of abdominal compression syndromes: The significance of hypermobility‐related disorders
- Nutcracker and May-Thurner syndrome: Decompression by extra venous tube grafting and significance of hypermobility related disorders
- Our surgical treatment of vascular compressions
- Chronic regional pain syndrome (CRPS) caused by venous compression and mechanical irritation of the coeliac plexus
- Vascular compression syndromes and other disease mechanisms I recently detected
- Kaleidoscope of instructive cases
- Venous congestion of the spinal cord may be a potential contributor to the development of paraplegia in patients with spinal muscular atrophy type III (Kugelberg-Welander disease)
- Ultrasound Diagnostics
- A breakthrough in functional sonographic diagnostic – 4D-colour Doppler sonographic flow volume measurements
- 4D-volume flow measurements of jugular and mesenteric veins
- Inauguration of the global volumetric brain perfusion measurement-a gateway for understanding of neurological symptoms
- Ultrasound focused entirely on all of your symptoms
- Ultrasound vs. X-ray
- Vascular Malformations
- Profile
- Functional colour Doppler ultrasound – how I do it
- Perfusion Measurement – PixelFlux-method
- Research
- Publications
- Nutcracker and May-Thurner syndrome: Decompression by extra venous tube grafting and significance of hypermobility related disorders
- Papers authored by Th. Scholbach
- Publications
- Inauguration of measurements of the tissue pulsatility index in renal transplants
- From nutcracker phenomenon to midline congestion syndrome and its treatment with aspirin
- First sonographic tissue perfusion measurement in renal transplants
- First sonographic bowel wall perfusion measurement in Crohn disease
- First sonographic renal tissue perfuison measurement
- First sonographic measurement of renal perfusion loss in diabetes mellitus
- PixelFlux measurements of renal tissue perfusion
- Why I prefer not to publish in journals but in the Internet
- Vessel stretching in nephroptosis – an important driver of complaints
- Publications
- Expertise
- Bornavirus Infection
- Scientific cooperation
- Cookie Policy
- Data protection
- Cookie Policy (EU)
- Impressum

A new variant of the left renal vein compression – compression by the left renal artery
Left renal vein compression is a common disease but little diagnosed. Some of the difficulties stem from the misleading name “Nutcracker syndrome”.
The term nutcracker syndrome was coined in 1972 by de Schepper, a Belgian radiologist ( de Schepper, A. “Nutcracker”-fenomeen van de vena renalis en veneuze pathologie van de linker nier. J Belge Radiol. 1972 Sep-Oct;55(5):507-11)
De Schepper found in patients with a haematuria that the left renal vein showed a significant narrowing while crossing the midline between the aorta and the superior mesenteric artery. Thus , the aorto-mesenteric fork resembling the 2 branches of a nutcracker prompted him to coin the term “Nutcracker syndrome”.
Unfortunately, the minority of the cases with a left renal vein compression show the compression exactly in front of the aorta.
Another little respected effect is often overseen. The superior mesenteric artery frequently deviates from the axis of the aorta. Thus, at the crossing of the left renal vein with the aorta the superior mesenteric artery often lies side-by-side to the aorta. In such a constellation a compression of the left renal vein by both arteries is impossible.
Many diagnostic errors occur when the diameter of the left renal vein in front of the aorta or in between the aorta-mesenteric fork is not or a little reduced. Then the diagnosis of a left renal vein compression is often falsely refuted.
It is thus necessary to be acquaint to the more frequent compression site of the left renal vein in front of the elbow like curvature of the right renal artery. In many cases the compression of the left renal vein is plus some millimetres to about 2 centimetres right to the aorta.
The fact that the increased lumbar lordosis is the underlying cause of all abdominal compression syndromes is not well known. The increased lumbar lordosis is producing a ventral displacement of the aorta thus squeezing the left renal vein from behind no matter if the superior mesenteric artery lies within the sagittal plane of the aortic axis or not.
Another consequence of a long-standing lumbar lordosis is an increased likelihood for the curvature of the spine to flip to the right side. The consequence is that the aorta is sliding towards the left of the spine. This stimulates a longitudinal clockwise twisting of the aorta if the vessel is seen from a caudal perspective.
This twisting significantly changes the orientation of the origin of the left and right renal artery. In most cases the left renal artery runs straight dorsally whereas the right renal artery runs at first ventrally but then curves dorsally to aim at the right kidney within the renal fossa.
Today I describe for the first time to the best of my knowledge the unusual compression of the left renal vein by the left renal artery.
In the affected patient the origin of the left renal artery was curved so that the left renal vein running in the same horizontal plane as the artery could become compressed.
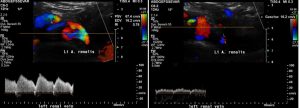
The left image shows the compression site of the left renal vein. The knee-like curvature of the left renal artery is squeezing from behind against the vein thus producing a significant pulsatile flow acceleration as can be seen in the spectral analyses on the bottom line. The yellow horizontal line is marking the centre of the aorta.
The right image shows that the flow pattern in in a more proximal portion of the left renal vein is not accelerated. Again, the yellow horizontal line is marking the Centre of the aorta. Thus, it can be clearly shown that the compression site of the left renal vein is downstream to the measurement site in this image.
In addition to this unusual left sided compression of the left renal vein the patient also had the common right sided compression in front of the right renal artery. Her symptoms consisted of bilateral suprainguinal pain increasing with the beginning of the menstruation. As in many other patients the left renal vein compression was accompanied by a May Thurner syndrome and a compression of the vena cava inferior by the exaggerated lordotic spine.